- Zahra Basirat
 - - Department of Obstet . and Gynecol Fateme Zahra Infertility Center, Shahid Yahyanejad Hospital, Babol University of Medical Science, Babol, Iran
- Nesa Asnafi
- - Department of Obstet . and Gynecol Fateme Zahra Infertility Center, Shahid Yahyanejad Hospital, Babol University of Medical Science, Babol, Iran
- Mehrdad Kashifard
- - Department of Internal Medicine, Ayat Allah Rouhani Hospital, Babol University of Medical Sciences, Babol, Iran
Received: 11/10/2009 Accepted: 2/17/2010 - Publisher : Avicenna Research Institute |
|
| Related Articles |
|
| Other Format |
|
|
|
Abstract
Introduction: Gestational diabetes is the most common metabolic disorder in pregnancy. Glucose Challenge Test (GCT) is done for all pregnant women during the 24th to 28th weeks of gestation. If the GCT value is more than 130 mg/dl a Glucose Tolerance Test (GTT) is asked and if GTT is impaired, gestational diabetes mellitus (GDM) is diagnosed and she will receive treatment accordingly. Some studies have illustrated that impaired GCT can cause unfavorable pregnancy outcomes. Therefore, the goal of this study was to determine the pregnancy outcome in pregnant women with abnormal GCTs. Materials and Methods: This study was done on all pregnant women attending Babol Shahid Yahyanezhad Hospital for prenatal care during 1999 to 2009. GCT was done for all the participants during the 24th to 28th weeks of gestation. Pregnancy outcomes of 225 pregnant women with abnormal GCTs and normal GTTs were compared with those of 225 pregnant women with normal GCTs as the controls. The individuals were compared for pregnancy outcomes such as macrosomia, premature rupture of membranes (PROM) and the need for a cesarean section (C/S). Results: The average birth weight of the neonates were 3.5 0.5 kg and 3.3 0.4 kg (p < 0.001) in the cases and controls, respectively. Twenty-five neonates in the case group (12.1%) and eight neonates in the control group (3.6%) had macrosomia (p = 0.003). Frequency of PROM was 17.85% (40) in the cases and 8.9% (20) in the controls (p = 0.008). The cases had a higher frequency for preeclampsia 4.4% (10) than the controls 1.8% (4), (p = 0.17). And pregnancy in the cases lead to a greater number of Cesarean sections, 42.2% (95) in comparison to the controls, 28% (63), (p < 0.001). Conclusion: Prevalence of macrosomia, PROM and C/S were higher in pregnant women with abnormal GCTs. Due to the aforementioned unfavorable conditions that bear the risk of a poor perinatal outcome, early diagnosis and proper follow up of women with GDM is suggested during the prenatal period.
Keywords:
Glucose intolerance, Glucose challenge test, Glucose tolerance test, Macrosomia, Preeclampsia, Pregnancy, Premature rupture of membrane To cite this article:Figures, Charts, Tables
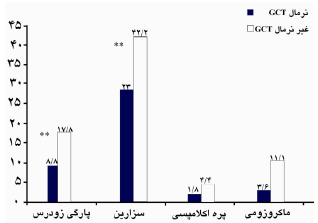
نمودار 1. مقایسه درصد پیامدهای نامطلوب بارداری در زنان باردار داراي GCT طبيعي و غيرطبيعي (GTT طبيعي)، مراجعهكننده به بیمارستان شهید یحیی نژاد بابل سال 88-87، (پیامد نامطلوب،* α =0/05معنیداری سطح،** α = 0/01 معنی داری سطح، *** α = 001/0 معنیداری سطح)
نمودار 1. مقایسه درصد پیامدهای نامطلوب بارداری در زنان باردار داراي GCT طبيعي و غيرطبيعي (GTT طبيعي)، مراجعهكننده به بیمارستان شهید یحیی نژاد بابل سال 88-87، (پیامد نامطلوب،* α =0/05معنیداری سطح،** α = 0/01 معنی داری سطح، *** α = 001/0 معنیداری سطح)
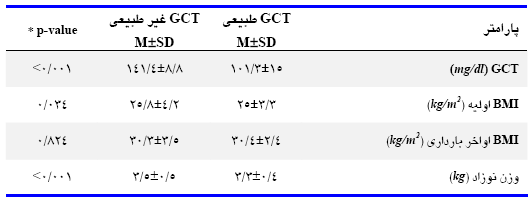
نمودار 1. مقایسه درصد پیامدهای نامطلوب بارداری در زنان باردار داراي GCT طبيعي و غيرطبيعي (GTT طبيعي)، مراجعهكننده به بیمارستان شهید یحیی نژاد بابل سال 88-87، (پیامد نامطلوب،* α =0/05معنیداری سطح،** α = 0/01 معنی داری سطح، *** α = 001/0 معنیداری سطح)
نمودار 1. مقایسه درصد پیامدهای نامطلوب بارداری در زنان باردار داراي GCT طبيعي و غيرطبيعي (GTT طبيعي)، مراجعهكننده به بیمارستان شهید یحیی نژاد بابل سال 88-87، (پیامد نامطلوب،* α =0/05معنیداری سطح،** α = 0/01 معنی داری سطح، *** α = 001/0 معنیداری سطح)
References
- Albert E. Diabetes mellitus and pregnancy. In: Ronald S, Beth Y, Arthur F, Ingrid N, editors. Danforths obstetrics and Gynecology. Philadelphia: A Wolters Kluwer Company; 2008. p. 246-50.
- Khoshnniat Nikoo M, Abbaszadeh Ahranjani S, Larijani B. A review on the prevalence of gestational diabetes mellitus (GDM) in different regions of Iran. Iran J Diabetes Lipid Disorders. 2009;8:7. [Abstract]
- Lurie S, Levy R, Weiss R, Boultin G, Hagay ZJ. Low values on 50 gram glucose challenge test or oral 100 gram glucose tolerance test are associated with good perinatal outcome. J Obstet Gynaecol. 1998;18(5):451-4. [PubMed]
- Retnakaran R, Qi Y, Sermer M, Connelly PW, Han-ley AJ, Zinman B. An abnormal screening glucose challenge test in pregnancy predicts postpartum metabolic dysfunction, even when the antepartum oral glucose tolerance test is normal. Clin Endocrinol (Oxf). 2009;71(2):208-14. [PubMed]
- Luengmettakul J, Boriboonhirunsam D, Sutantawibul A, Sunsaneevithayakul P. Incidence of large-for-gestational age newborn: a comparison btween pregnant women with abnormal and normal screeing test for gestational diabetes. J Med Assoc Thai. 2007;90(3):432-6. [PubMed]
- Ronald S. Premature Rupture of the Membranes. In: Ronald S, Beth Y, Arthur F, Ingrid N, editors. Danforths obstetrics and Gynecology. Philadelphia: A Wolters Kluwer Company; 2008. p. 186-95.
- Mounira H, Baha M. Hypertensive disorders of pregnancy. In: Ronald S, Beth Y, Arthur F, Ingrid N, editors. Danforths obstetrics and Gynecology. Philadelphia: A Wolters Kluwer Company; 2008. p. 258.
- Cunnigham FG, Leveno KJ, Bloom SL, Hauth JC, Gilstrap LC, Westrom KD. William's Obstetrics. 22nd ed. USA: Mc Graw Hill; 2005. Chapter 52, diabetes; p. 1170-84.
- Kim HS, Chang KH, Yang JI, Yang SC, Lee HJ, Ryu HS. Clinical outcomes of pregnancy with one elevated glucose tolerance test value. Int J Gynaecol Obstet. 2002;78(2):131-8. [PubMed]
- Yogev Y, Langer O, Xenakis EM, Rosenn B. The association between glucose challenge test, obesity and pregnancy outcome in 6390 non-diabetic women. J Matern Fetal Neonatal Med. 2005;17(1): 29-34. [PubMed]
- Chu SY, Callaghan WM, Kim SY, Schmid CH, Lau J, England LJ, et al. Maternal obesity and risk of gestational diabetes mellitus. Diabetes Care. 2007;30(8):2070-6. [PubMed]
- Mello G, Parretti E, Mecacci F, Lucchetti R, Lagazio C, Pratesi M, et al. Risk factors for fetal macrosomia: the importance of a positive oral glcose challenge test. Eur J Endocrinol. 1997;137(1):27-33. [PubMed]
- Bevier WC, Fischer R, Jovanovic L. Treatment of women with an abnormal glucose challenge test (but a normal oral glucose tolerance test) decreases the prevalence of macrosomia. Am J Perinatol. 1999;16(6):269-75. [PubMed]
- Lin CH, Wen SF, Wu YH, Huang MJ. Using the 100-g oral glucose tolerance test to predict fetal and maternal outcomes in women with gestational diabetes mellitus. Chang Gung Med J. 2009;32(3): 283-9. [PubMed]
- Jolly MC, Sebire NJ, Harris JP, Regan L, Robinson S. Risk factors for macrosomia and its clinical cosequences: a study of 350, 311 pregnancies. Eur J Obstet Gynecol Reprod Biol. 2003;111(1):9-14. [PubMed]
- Sebire NJ, Jolly M, Harris JP, Wadsworth J, Joffe M, Beard RW, et al. Maternal obesity and pregnancy outcome: a study of 287, 213 pregnacies in London. Int J Obes Relat Metab Disord. 2001;25 (8):1175-82. [PubMed]
- Thanasuan S, Borriboonhirunsarn D. Incidence of gestational diabetes mellitus among pregnant women with one abnormal value of oral glucose tolerance test. J Med Assoc Thai. 2006;89(8):1109-14. [PubMed]
- Sun WJ, Yang HX. [Maternal and fetal outcomes in pregnant women with abnormal glucose metabolism]. Zhonghua Fu Chan Ke Za Zhi. 2007;42(6): 377-81. Chinese. [PubMed]
- Dudhbhai M, Lim L, Bombard A, Juliard K, Meenakshi B, Trachelenberg Y, et al. Characteriics of patients with abnormal glucose challenge test and normal oral glucose tolerance test results: comparison with normal and gestational diabetic patients. Am J Obstet Gynecol. 2006;194(5):e42-5. [PubMed]
- Yang HX, Zhang MH, Sun WJ, Dong Y. [Associated factors of preeclampsia complicated in prenant women with abnormal glucose metabolism]. Zhonghua Fu Chan Ke Za Zhi. 2005;40(9):577-80. Chinese. [PubMed]
- Luengmettakul J, Boriboonhirunsam D, Sutantawibul A, Sunsaneevithayakul P. Incidence of largefor-gestational age newborn: a comparison btween pregnant women with abnormal and normal screening test for gestational diabetes. J Med Assoc Thai. 2007;90(3):432-6. [PubMed]